
ENSURING
DIABETIC
FOOT CARE @ AFFORDABLE
COST
Amputation
is not an
answer to diabetic foot
Paadavinyas
A training program in Diabetic Foot and Preventive Podiatry since 2013. Aim is to impart training in Diabetic Foot and preventive podiatry to the primary care physicians of Govt.Hospitals and
Primary Health centres.
Take Care of your Feet just like your Face !
- Take care of your Feet on a daily basis
- Proper Foot wear
- Inspection of Feet at bed time
- Nail cutting
- Weekly Pedicure

“Treat each and every individual with dignity and mutual respect”

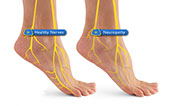
How can diabetes affect your feet?
Living with diabetes requires you to pay special attention to your health and your condition. Keeping your blood sugar (glucose) levels within the recommended range is one of the best things you can do to control your condition and protect your feet.Chronically high blood sugar (glucose) levels can be associated with serious complications in people who have diabetes. The feet are especially at risk. Two conditions called diabetic neuropathy and peripheral vascular disease can damage the feet (and other areas of the body) in people who have diabetes.
Diabetic neuropathy
Chronically high sugar levels associated with uncontrolled diabetes can cause nerve damage that interferes with the ability to sense pain and temperature. This so-called "sensory diabetic neuropathy" Nearly 10% of people with diabetes develop foot ulcers due to peripheral vascular disease and nerve damage. People with diabetes may not notice sores or cuts on the feet, which in turn can lead to an infection. Nerve damage can also affect the function of foot muscles, leading to improper alignment and injury.
Peripheral vascular disease
Diabetes is associated with poor circulation (blood flow). Inadequate blood flow increases the healing time for cuts and sores. Peripheral vascular disease refers to compromised blood flow in the arms and legs. Poor blood flow increases the risk that infections will not heal. This, in turn, increases the risk of ulcers and gangrene, which is tissue death that occurs in a localized area when there is an inadequate blood supply.
Common foot problems of people with diabetes
If you have diabetes, the common foot problems below can lead to pain or infections that make it hard to walk. If you have any of these problems, make sure you get prompt treatment from your doctor.
Corn and callus
Corns and calluses are thick layers of skin.
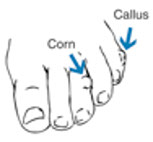
- Corns and calluses are caused by too much rubbing or pressure on the same spot. They often form where the first and second toes overlap.
- You can gently rub a pumice stone on a corn or callus after you take a bath or shower to wear it down. A pumice stone is a type of rock used to smooth the skin. However, check with your doctor about the best way to care for a corn or callus.
- If an infection occurs in an area of a corn or callus, your doctor may need to remove the unhealthy tissue and give you antibiotics.
Blister
Blisters are areas of skin that are raised and filled with fluid.
- A blister can form if your shoe always rubs the same spot on your foot.
- Wearing shoes that do not fit or wearing shoes without socks also can cause blisters.
- To prevent a blister, use socks or a bandage over the spot being rubbed. Wear shoes that fit properly.
- Cover small blisters with a bandage, and cover large ones with a gauze pad held with adhesive or paper tape. You also can buy special blister bandages in different sizes at a drugstore.
- If your blister is infected, your doctor may need to drain the fluid from the blister and give you antibiotics.
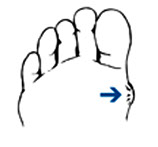
Ingrown toenail
Ingrown toenails happen when the edges of your toenails grow into your skin
- Ingrown toenails can form if you wear shoes that are too tight or cut into the corners of your toenails when you trim them.
- To prevent ingrown toenails, wear shoes that fit properly.
- If your toenail edges are sharp, smooth them with a nail file or emery board instead of cutting them.
- If you go to a salon for a pedicure, make sure they do not cut into the corners of your toenails. Never treat ingrown toenails at home. Your doctor may remove part of your toenail to help it heal or keep it from growing back into your skin. If your toe is infected, you may need antibiotics.
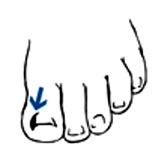
Bunion
A bunion is a bump at the outside edge of your big toe. As the bump gets worse, it can be filled with extra bone and fluid.
- Bunions form when your big toe slants toward your small toes. High heels, pointed shoes, or shoes that are too tight or narrow may cause bunions. Bunions often run in families.
- To prevent bunions, wear shoes that fit well.
- Use padded shoe inserts to prevent a bunion from getting worse and using medicine to reduce pain and swelling. You may need surgery to remove a bunion that causes frequent pain.
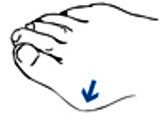
Plantar warts
Plantar warts are small, flesh-colored growths on the bottoms of your feet. Sometimes you see tiny, black dots in the warts.
- Plantar warts are caused by a virus that enters your feet through small breaks in your skin. The warts can be painful and make it hard to walk.
- To prevent plantar warts from spreading, avoid contact with your warts and wash your hands after touching them.
- Keep your feet clean and dry.
- Don’t go barefoot in public areas.
- Remove plantar warts with minor surgery, laser treatment, liquid nitrogen, or medicines.
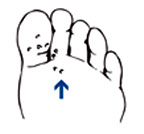
Hammertoe
Hammertoes are toes that curl under your feet
- Hammertoes form when one or both joints of the small toes bend from weakness in your foot muscle. Diabetic nerve damage may cause the weakness.
- You may get sores on the bottoms of your feet and on the tops of your toes that can become infected.
- The shape of your feet may change.
- You can have problems walking and finding shoes that fit well.
- Avoid high heels or shoes with pointed toes.
- Medicines can reduce pain and swelling. If your hammertoe becomes rigid and painful, or if an open sore has formed, you may need surgery to correct your toe.
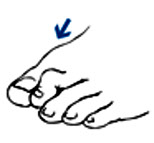
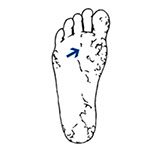
Dry and cracked skin
Dry and cracked skin is rough, scaly, and flaking. Your skin may be gray if you have dark skin. Your skin may be red or itch.
- Dry and cracked skin can be caused by high blood glucose, nerve damage, or poor blood flow.
- Cracks allow infection to start.
- Keep your feet moist with lotion or petroleum jelly.
- Do not soak your feet because your skin could become drier.
- If you cannot treat your dry and cracked skin at home, see your doctor. You may need a prescription ointment or cream.
- To prevent athlete’s foot, keep your feet as dry as you can.
- Try not to wear the same shoes all the time. Try to wear socks that do not trap moisture, such as cotton or wool socks.
- Wear waterproof shoes or flip-flops in public showers.
- If you go to a salon for a pedicure, ensure the tools are sterilized or bring your own tools.
- See your doctor to make sure you have athlete’s foot. You can buy sprays and creams to treat fungus at a drugstore; however, your doctor may prescribe a stronger oral medicine.
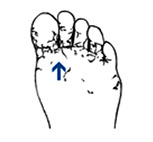
Athlete’s foot
Athlete’s foot is a fungus that causes itching, burning, redness, and cracking of your skin. The fungus grows on the soles of your feet and in between your toes.
Fungal infection
Fungal infection of the toenails makes them thick, hard to cut, and appear yellow, green, brown, or black. A nail may also fall off.
- To prevent a fungal infection of the toenails, keep your feet as dry as you can.
- Try not to wear the same shoes all the time. Try to wear socks that do not trap moisture, such as cotton or wool socks.
- Wear waterproof shoes or flip-flops in public showers.
- If you go to a salon for a pedicure, ensure the tools are sterilized or bring your own tools.
- See your doctor to make sure you have a fungal infection of the toenails. Your doctor may prescribe an oral medicine to treat them. Sometimes, a doctor may remove the nail surgically or chemically or perform laser treatment. A laser beam can go deep into the nail tissue and kill the fungus; however, doctors are still studying how well this treatment works.
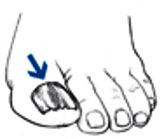
Risk Factors for Diabetic Foot Ulcers
All people with diabetes are at risk for foot ulcers, which can have multiple causes. Some factors can increase the risk of foot ulcers, including:
- poorly fitted or poor quality shoes
- poor hygiene (not washing regularly or thoroughly)
- improper trimming of toe nails
- alcohol consumption
- tobacco use (inhibits blood circulation)
No Diabetic Foot Ulcerates Spontaneously...
-
- High risk foot is a foot that has developed one or more of the following risk factors for ulceration:
- Neuropathy
- Ischaemia
- Deformity
- H/O previous ulceration
@ 2016 Ajaiyakumar, Thiruvanathapuram



